Plantar fasciitis hits you hardest on that first step out of bed—sharp, stabbing pain where your heel meets the arch. You’re dealing with tiny tears and wear on the thick band of tissue supporting your foot’s arch, not just inflammation. It’s common; roughly one in ten people get it, especially between forty and sixty. Rest, ice, stretching, and supportive shoes tackle most cases. The good news? You’ve got solid options beyond what you’re trying now.
Key Takeaways
- Plantar fasciitis causes sharp heel pain from microtears and degeneration of the plantar fascia, a thick band supporting the arch.
- Characteristic “first-step pain” occurs after rest periods like waking up or prolonged sitting, then typically eases with activity.
- Clinical diagnosis relies on history and physical exam findings; imaging is generally unnecessary for typical presentations.
- Conservative treatment includes rest, ice, daily stretching, supportive footwear, orthotics, and night splints for persistent cases.
- Prevention strategies involve regular calf and plantar fascia stretching, proper arch support, gradual activity increases, and maintaining healthy body weight.
What Is Plantar Fasciitis?
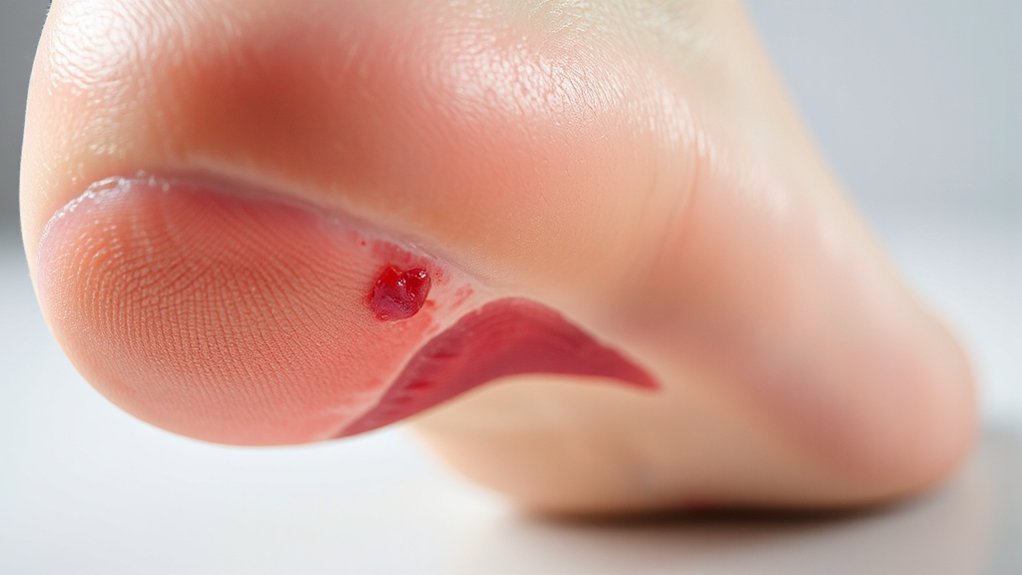
Plantar fasciitis is heel pain caused by injury and wear-and-tear of the plantar fascia—that thick, fibrous band running from your heel bone down to your toes that basically holds your foot arch together. You’re dealing with microtears and degeneration, not just inflammation. It’s the most common source of heel pain, affecting roughly 1 in 10 people during their lifetime, typically hitting hardest between ages 40 and 60.
Here’s what’s happening: repeated tension and stretching cause the fascia to thicken and deteriorate over time. You’ll notice focal tenderness right where your heel connects to that fibrous band. Risk factors stack up if you’re standing constantly, carrying extra weight, running regularly, or sporting naturally high arches or flat feet. Your foot mechanics matter more than you’d think. The condition develops gradually, making early attention vital for avoiding prolonged discomfort.
Plantar Fasciitis Symptoms: When and Where Pain Strikes

Where does it hurt, and when does it hurt worst?
You’ll feel it right there—sharp, stabbing pain at your heel’s inner edge where the plantar fascia attaches. That’s your medial calcaneal tuberosity, and yeah, it’s tender.
The real kicker? First-step pain. You roll out of bed or stand after sitting, and—ouch—that initial push off your toes feels awful. Give it a few minutes though. The pain typically eases as you warm up and walk around.
First-step pain is the real kicker—that initial push off your toes hurts, but it eases as you warm up and walk around.
But here’s the catch: it often returns after prolonged standing, long walks, or intense activity. Notice the pattern—pain hits *after* exercise, not during it.
You might experience this one-sided, though about 30% of people deal with it both feet. Hard, unsupportive surfaces and certain movements (like toe dorsiflexion) trigger flare-ups. Your plantar fascia’s tightness, unfortunately, makes every step a potential negotiation.
How Do Doctors Diagnose Plantar Fasciitis?
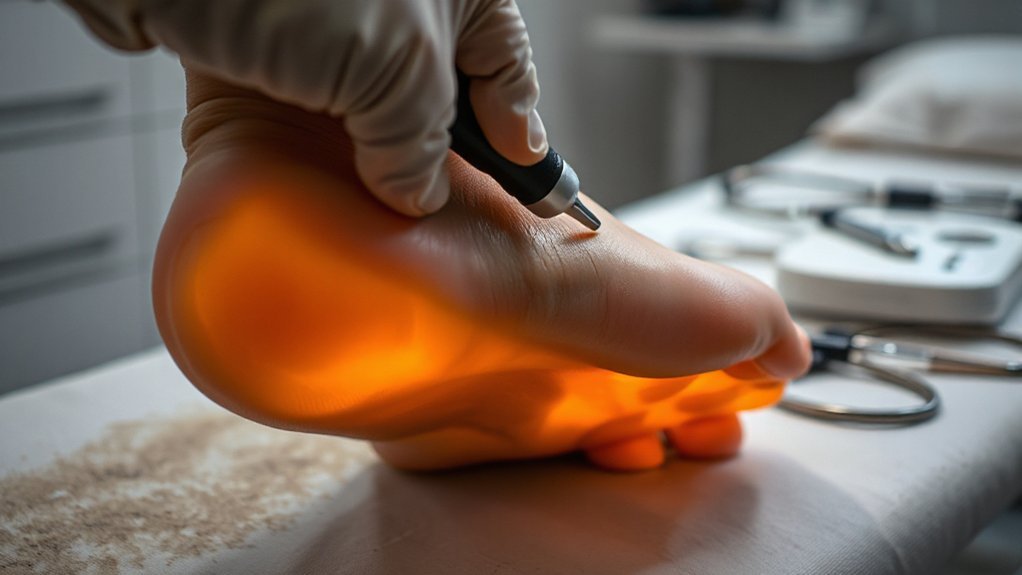
How’s your doctor actually going to figure out if you’ve got plantar fasciitis? Honestly, they’ll start with what you tell them. They’ll ask about that first-step pain when you roll out of bed, how it eases up after walking, then comes back with prolonged standing. That history matters more than you’d think.
Then comes the physical exam. Your doctor will press on your heel’s inner edge—right where the plantar fascia attaches—and watch you wince. They’ll have you pull your toes upward or stand on your tiptoes, checking if that triggers pain. They’re also checking your calf tightness and overall foot posture.
Imaging? Usually unnecessary. X-rays or ultrasound come into play only when your pain sticks around despite treatment or when something feels off about your presentation. Most times, that clinical picture—your symptoms plus exam findings—tells your doctor everything they need.
Treating Plantar Fasciitis: Home Care to Surgery
Since most people get better without ever setting foot in an operating room, here’s the thing: you’ve got plenty of weapons before surgery even enters the conversation. Start with the basics—rest, ice for 10–15 minutes twice daily, stretching your plantar fascia and calves daily, plus over-the-counter NSAIDs when pain flares. Supportive shoes and temporary orthotics or heel cups take pressure off your arch. Night splints work surprisingly well for that brutal morning first step, especially if symptoms linger beyond six months. Most folks improve within weeks to months with these moves alone. If that doesn’t cut it, your doctor might suggest corticosteroid injections for short-term relief or shockwave therapy for stubborn cases. Surgery? That’s your last resort after six to twelve months of serious conservative care. It works, but only when nothing else does.
Preventing Plantar Fasciitis and Stopping Recurrence
Getting better’s the victory—staying better’s the real test. Here’s what actually works: stretch your plantar fascia and calves daily, aim for three minutes three times or five 20-second stretches twice daily. Sounds simple? It prevents recurrence. Wear shoes with solid arch support and cushioning; ditch the barefoot walks on hard floors. Replace running shoes every 250–500 miles.
During flare-ups, use arch supports or heel cups for up to three months—they’re your temporary bodyguards. Don’t jump into intense activity; follow the 10% rule for weekly increases, and cross-train with swimming or cycling instead.
Here’s the honest part: losing excess weight reduces plantar load substantially. Address calf tightness through physical therapy if needed. These aren’t flashy fixes, but they’re what actually stops pain from creeping back. You’ve got this.
Frequently Asked Questions
How Long Does Plantar Fasciitis Typically Take to Heal Completely?
You’re typically looking at three to twelve months for complete healing, though most folks see real improvement in six to eight weeks with consistent treatment. Here’s the thing: you’ve got to be patient and proactive. Ice it, stretch regularly, wear supportive shoes, and consider night splints. Skip the running marathons while you’re healing. Stick with it—your feet’ll thank you.
Can Plantar Fasciitis Develop in Both Feet Simultaneously or Just One?
You can definitely develop plantar fasciitis in both feet—studies show about 10% of people experience it bilaterally. Here’s the thing: your body often compensates when one foot hurts, shifting weight and stressing the other. You’re basically limping your way toward a matching pair of problems. The good news? Treating both simultaneously with stretches, proper footwear, and ice actually works better than managing solo pain. Prevention’s your best friend here.
What Is the Success Rate of Shockwave Therapy for Plantar Fasciitis?
You’re looking at roughly 65-70% success rates with extracorporeal shock wave therapy—pretty solid odds, honestly. Here’s the thing: it works best when you’ve already tried stretching, rest, and orthotics for months without relief. Your body needs those sound waves to break up scar tissue and spark healing. Some folks see results in weeks; others need multiple sessions. Insurance might balk, but many consider it worth exploring before surgery.
Is Plantar Fasciitis Hereditary or Does It Run in Families?
Your family’s footprint—literally—might matter here. While you won’t inherit plantar fasciitis outright, you can inherit the problematic physical traits that prompt it: flat feet, tight calves, or biomechanical imbalances. Your parents’ foot structure often becomes yours. So if your relatives wrestled with heel pain, you’re predisposed, not predetermined. You’ve still got control through stretching, proper footwear, and preventive care. Genes load the gun; your habits pull the trigger.
Can Children Develop Plantar Fasciitis or Is It Only Adults?
You’d think kids are immune to foot pain, right? They’re not. Children can develop plantar fasciitis, though it’s less common than in adults. You’ll typically see it in active kids—especially those doing sports like soccer or running. Growth spurts, tight calf muscles, and flat feet increase risk. If your child complains about heel pain during activity, don’t dismiss it. Getting early treatment prevents worse problems down the road.
So
You’ve got this. Whether you’re a runner who ignored that morning twinge or someone who finally decided heel pain doesn’t have to be your normal, you can beat plantar fasciitis. Start with stretches, proper shoes, maybe ice. Most people see relief in weeks, not months. Stay consistent, listen to your feet, and you’ll reclaim those pain-free mornings you’ve been missing.






Leave a Comment